According to The Conversation, almost 1 million people die every year from bacterial infections. The rise of superbugs–antibiotic resistant bacteria–is attributed to the misuse of antibiotics which allows bacteria to alter the ways antibiotics once targeted them, preventing them from working. Below are two antibiotic resistant organisms that pose a serious health threat to society.
1. Klebsiella pneumoniae
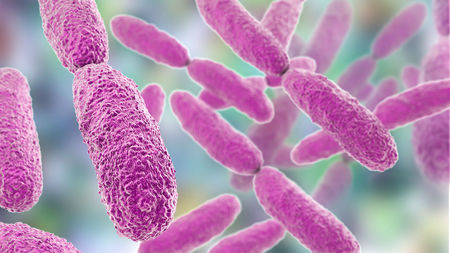
Klebsiella pneumoniae is an encapsulated gram-negative enterobacterium that is associated with carbapenam resistant enterobacteria (CRE). According to Nature, carbapenam resistant Klebsiella pneumoniae (CRKP) is resistant to all b-lactam antibiotics making it one of the leading bacterial pathogens causing hospital-associated infections. Up until 2001, carbapenams were used as last-resort option for treating multi-drug resistant K. pneumoniae. This was before the first discovery of the production of K. pneumoniae carbapenemase (KPC) in isolated colonies in North Carolina (shout out NC). Since then, CRKP is found throughout the world. According to The Conversation, in 2013, 8,000 cases of multi-drug resistant K. pneumoniae were reported in the United States alone with a 50% death rate for bloodstream infections. In 2016, a strain of K. pneumoniae was found to be resistant to 26 antibiotics making this bacteria pandrug-resistant. The patient with this strain died due to lack of alternative treatments. This is not an isolated case as more bacteria are becoming pandrug-resistant. This presents a serious health threat for discovering alternative solutions for treating this infection.
2. Methicillin Resistant Staphylococcus aureus (MRSA)
Staphylococcus aureus is a gram-positive bacterium that quickly became another one of the leading bacterial pathogens to cause hospital-associated infections. According to Nature, penicillin was first used to treat S. aureus but was a short-lived solution as it developed resistance to penicillin in the 1940s. The first semi-synthetic versions of penicillin were created around 1960 and methicillin resistant S. aureus developed after 1 year of the first clinical use. MRSA was first discovered in the 1960s from clinically isolated patients in the hospital but since the 1990s, MRSA has spread throughout the community. In another news report from The Times of India, MRSA is spreading into the milk, poultry, and fish products of Gujarat. The prevalence of MRSA comes from the use and abuse of antimicrobials in human, animal, and environmental sectors.
The prevalence of MRSA around the world poses a serious health threat. So the question is, how do we prevent increased antibiotic resistance? Personally, I think there is a lot to blame on the doctors that over prescribe antibiotics like they’re candy. If this problem is going to be fixed then it is in the hands of the healthcare providers that treat such diseases to know when it is absolutely necessary to use such antibiotics. If this problem is never fixed, we very well may no longer have treatments for life-threatening diseases.
“To fight antibiotic resistance, we need coordinated action in society.”
Dr. Bhavini Shah from The Times of India
